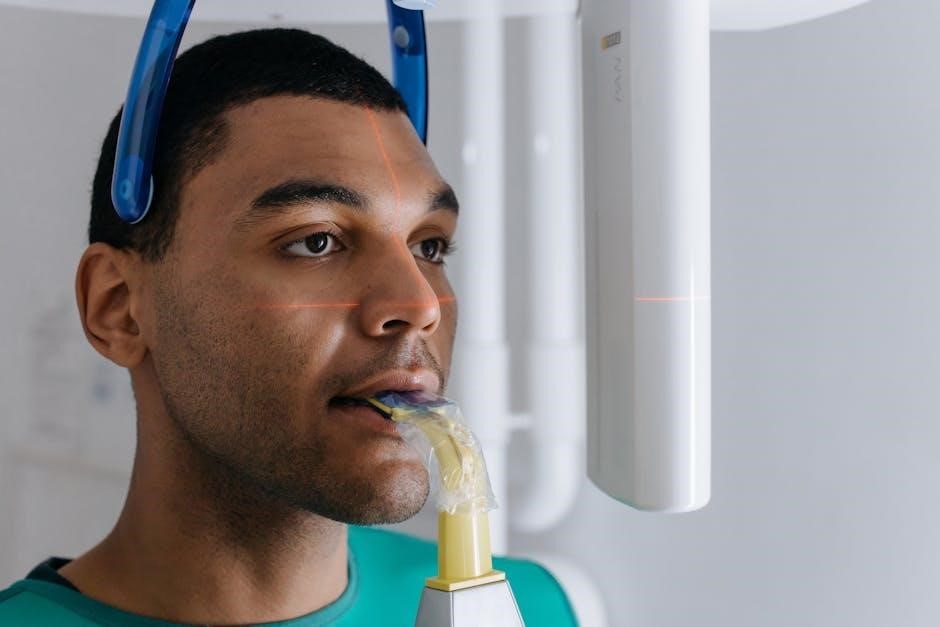
Proper patient positioning is essential for safe and successful surgery. It ensures optimal access to the surgical site while minimizing physiological compromise and preventing positioning-related injuries like nerve damage and pressure ulcers.
Importance of Proper Patient Positioning
Optimal patient positioning during surgical and other invasive procedures is paramount for several critical reasons. First and foremost, it provides the surgeon with unobstructed access to the operative site, enabling them to perform the procedure efficiently and effectively. Good surgical access is essential for visualization and manipulation, contributing directly to a successful outcome. Secondly, proper positioning is crucial for maintaining the patient’s physiological well-being. Thoughtful positioning promotes circulation and respiratory function, minimizing the risk of complications such as hypoxemia or venous stasis. It also protects bony prominences and minimizes nerve pressure, preventing potential nerve damage and pressure ulcers. Furthermore, correct positioning ensures patient comfort and dignity throughout the procedure. Healthcare workers should always consider patient comfort, safety, and minimizing risk of injury and promote safe work practices during patient handling tasks. Improper positioning, on the other hand, can lead to a range of adverse outcomes, including nerve injuries, pressure ulcers, compromised respiratory function, and circulatory problems. Therefore, a thorough understanding of positioning principles and the use of appropriate equipment and techniques are vital for all perioperative team members. Ultimately, proper patient positioning is a cornerstone of safe and effective perioperative care, contributing significantly to positive patient outcomes and a reduction in potential complications. It allows secure access to the surgical site with the least physiological compromise to the patient.
Principles of Safe Patient Positioning
Safe patient positioning relies on key principles. These include maintaining neutral alignment, protecting pressure points, ensuring adequate circulation and respiration, and understanding the specific needs of vulnerable patients, like those who are obese or pregnant.
Maintaining Neutral Head and Neck Alignment
Maintaining neutral head and neck alignment is paramount in patient positioning to prevent brachial plexus injury. This involves ensuring the head is neither excessively flexed, extended, rotated, nor laterally bent. Proper alignment reduces the risk of nerve compression and subsequent neurological deficits. Perioperative team members must meticulously assess and adjust the patient’s head and neck position throughout the procedure. Use supportive devices like gel pads or specialized headrests to maintain the desired alignment. Regularly reassess the position to prevent pressure points on the scalp and subsequent skin breakdown. Consider the patient’s individual anatomical variations and any pre-existing conditions that may affect their susceptibility to nerve injury. Communication among the surgical team is crucial to ensure everyone is aware of the importance of maintaining neutral head and neck alignment. Document the positioning techniques and any devices used to maintain alignment. The AORN guideline emphasizes the importance of this principle for all surgical positions. Implementing these practices can significantly decrease the risk of brachial plexus injury and improve patient outcomes. Proper documentation is key to ensure quality care. Remember to reposition the patient’s head periodically to alleviate pressure. Patient safety remains the top priority;

Common Surgical Positions
Surgical positions vary based on the procedure, with common ones including supine, prone, and lithotomy. Each position presents unique considerations for patient safety and physiological impact. Careful planning and execution are essential for optimal outcomes.
Supine Position
The supine position, also known as the dorsal decubitus position, involves the patient lying flat on their back with the face upward. This is one of the most frequently used positions in surgery, providing access to the anterior surface of the body, including the abdomen, chest, and anterior extremities. When positioning a patient in the supine position, it’s crucial to ensure proper alignment of the head, neck, and spine to prevent nerve damage, particularly to the brachial plexus. The head should be maintained in a neutral position, avoiding excessive rotation or extension. Padding should be placed under the head, if necessary, to maintain alignment and prevent pressure on the occiput. The arms can be positioned in several ways, depending on the surgical site and the patient’s anatomy. They can be tucked at the patient’s sides, secured on arm boards at a 90-degree angle, or extended overhead. When extending the arms, care must be taken to avoid hyperextension of the shoulder joint, which can lead to nerve injury. Padding should be placed under the elbows and wrists to protect bony prominences. The legs should be slightly bent at the hips and knees to reduce pressure on the lumbar spine. A small pillow or pad can be placed under the knees to further alleviate pressure. The ankles should be supported to prevent plantar flexion and potential foot drop. A body strap can be used to secure the patient to the operating table, ensuring their safety throughout the procedure. It’s important to monitor pressure points and skin integrity throughout the surgery, repositioning the patient as needed to prevent pressure ulcers. Special considerations should be taken for patients who are pregnant or obese, as their anatomical differences may require additional padding and support to maintain proper alignment and prevent complications. The supine position is versatile but demands meticulous attention to detail to ensure patient safety and comfort.
Prone Position
The prone position involves the patient lying face down with the chest and hips supported by specialized pads or frames. This position is commonly used for surgical procedures involving the posterior aspect of the body, such as the spine, back of the head, and certain lower extremity procedures. Achieving and maintaining a safe prone position requires careful attention to detail to prevent complications such as pressure ulcers, nerve injuries, and respiratory compromise. When transitioning a patient to the prone position, it’s essential to ensure that the head and neck are properly aligned to avoid excessive rotation or flexion, which can lead to brachial plexus injury or other nerve damage. The head is typically supported by a horseshoe-shaped headrest or a gel pad, allowing the face to be free from pressure. The arms can be positioned in several ways, depending on the surgical site and patient factors. They can be placed alongside the head, extended overhead, or tucked at the patient’s sides. Regardless of the arm position, it’s crucial to ensure that the shoulders are not excessively abducted or rotated, as this can also contribute to nerve injury. The chest and hips should be supported by specialized prone positioning pads or frames, such as the Wilson frame or the Andrews frame, to allow for adequate ventilation and reduce pressure on the abdomen. These frames elevate the abdomen, decreasing pressure on the inferior vena cava and improving venous return. The legs should be slightly flexed at the knees, and padding should be placed under the ankles to prevent pressure on the bony prominences. It’s important to regularly assess the patient’s skin for signs of pressure and to reposition them as needed to prevent pressure ulcers. Special consideration should be given to patients who are obese or have respiratory compromise, as the prone position can further restrict lung expansion. Close monitoring of respiratory status is essential throughout the procedure. The prone position, while necessary for certain surgeries, requires meticulous attention to detail and careful planning to ensure patient safety and minimize potential complications.
Lithotomy Position
The lithotomy position involves the patient lying on their back with their legs raised and abducted, typically supported by stirrups. This position is commonly used for gynecological, urological, and rectal surgeries. Proper execution of the lithotomy position is crucial to prevent nerve injuries, circulatory compromise, and other complications. When positioning a patient in the lithotomy position, it’s essential to ensure that the hips and knees are flexed appropriately and that the legs are symmetrically positioned in the stirrups. The angle of hip flexion and knee flexion should be determined based on the patient’s individual anatomy and the requirements of the surgical procedure. It’s important to avoid excessive hip flexion, as this can compress the femoral nerve and lead to postoperative neuropathy. The stirrups should be padded to protect the patient’s legs and ankles from pressure. The height of the stirrups should be adjusted to ensure that the legs are not excessively elevated or lowered, as this can affect venous return and increase the risk of deep vein thrombosis (DVT). The arms should be carefully positioned to avoid nerve compression. They can be placed alongside the body, tucked at the patient’s sides, or extended on arm boards. Regardless of the arm position, it’s crucial to ensure that the shoulders are not excessively abducted or rotated, as this can contribute to brachial plexus injury. The duration of time spent in the lithotomy position should be minimized whenever possible to reduce the risk of complications. If the procedure is expected to be lengthy, it’s important to periodically assess the patient’s circulation and nerve function in the legs and feet. Special consideration should be given to patients who have pre-existing vascular disease or neuropathy, as they may be at increased risk for complications. The lithotomy position, while necessary for certain surgeries, requires careful attention to detail and meticulous planning to ensure patient safety and minimize potential complications such as nerve damage and circulatory issues.

Potential Injuries Related to Improper Positioning
Improper patient positioning during surgical procedures can lead to nerve damage and pressure ulcers. Vigilance in maintaining neutral alignment and relieving pressure on bony prominences is crucial for prevention.
Nerve Damage
Nerve damage is a significant risk associated with improper or prolonged patient positioning during surgical procedures. The brachial plexus, in particular, is vulnerable if the head and neck are not maintained in a neutral position. Excessive stretching, compression, or direct pressure on nerves can result in temporary or permanent neurological deficits. Peripheral nerves are also susceptible to injury from prolonged pressure against hard surfaces, especially in areas where they are close to bony prominences. Factors such as patient size, pre-existing conditions (e.g;, diabetes, neuropathy), and the duration of the surgical procedure can increase the risk of nerve damage. Careful attention to positioning techniques, including the use of appropriate padding and support devices, is essential to minimize the risk of nerve compression and stretching. Regular assessment of the patient’s extremities for signs of impaired circulation or neurological function should be performed throughout the procedure. Communication among the surgical team members regarding potential positioning-related risks is crucial to ensure patient safety. Perioperative nurses play a vital role in advocating for the patient and ensuring that positioning guidelines are followed meticulously. Neurological deficits can manifest as numbness, tingling, weakness, or paralysis, and can significantly impact the patient’s postoperative recovery and quality of life. Therefore, preventive measures are paramount to minimize the incidence of nerve damage related to patient positioning.
Pressure Ulcers
Pressure ulcers, also known as bedsores or pressure injuries, represent a significant risk for patients undergoing surgical procedures, particularly those involving prolonged positioning. These localized injuries to the skin and underlying tissue typically occur over bony prominences due to sustained pressure, shear forces, and friction. The sacrum, heels, elbows, and ischial tuberosities are common sites for pressure ulcer development. Several factors contribute to the risk of pressure ulcer formation, including patient immobility, advanced age, compromised nutritional status, impaired circulation, and underlying medical conditions such as diabetes and vascular disease. Prolonged pressure reduces blood flow to the affected area, leading to tissue ischemia and eventual necrosis. Shear forces, which occur when layers of tissue slide against each other, can further damage blood vessels and contribute to tissue breakdown. Friction, caused by rubbing against surfaces, can also damage the skin’s protective barrier. Preventive measures are crucial to minimize the risk of pressure ulcer development. These include frequent repositioning of the patient, the use of pressure-redistributing support surfaces (e.g., specialized mattresses, gel pads), meticulous skin care, and adequate nutritional support. Regular assessment of the patient’s skin for signs of redness, blanching, or breakdown is essential. Proper positioning techniques that distribute weight evenly and minimize pressure on bony prominences are paramount. Perioperative nurses play a critical role in identifying patients at risk for pressure ulcers and implementing appropriate preventive strategies. Early detection and intervention are key to preventing the progression of pressure ulcers and minimizing their impact on patient outcomes. The RNAO best practice guidelines, Assessment and Prevention of Pressure provide valuable guidance.

Equipment and Materials for Safe Positioning
Safe patient positioning during surgical procedures relies heavily on the appropriate selection and utilization of specialized equipment and materials. These tools are designed to support the patient’s body, maintain proper alignment, and minimize the risk of pressure injuries and nerve damage. A wide array of devices is available to accommodate various surgical positions and patient needs. Pressure-redistributing mattresses and overlays are fundamental for reducing pressure on bony prominences; These surfaces are often made of foam, gel, or air-filled materials that conform to the patient’s body and distribute weight evenly. Gel pads and foam cushions are used to protect specific areas, such as the heels, elbows, and sacrum. Headrests and supports are essential for maintaining neutral head and neck alignment, preventing brachial plexus injuries. Arm boards and supports are used to secure the arms in a safe and comfortable position, avoiding excessive abduction or extension. Body straps and tape can be used to stabilize the patient on the operating table, particularly in positions that require a degree of tilt or rotation. However, care must be taken to avoid constricting circulation or causing pressure on nerves. Specialized positioning devices, such as beanbags, wedges, and rolls, can be used to achieve specific angles and support the patient in various positions. For example, beanbags can be molded to conform to the patient’s body, providing customized support and stability. Stirrups are used in the lithotomy position to support the legs, and they come in various styles to accommodate different patient sizes and surgical needs. Anti-Stat Patient Shifters are used to safely transfer patients. The selection of appropriate equipment should be based on a thorough assessment of the patient’s individual needs, the planned surgical procedure, and the desired position. Perioperative nurses play a crucial role in selecting and utilizing positioning equipment effectively to ensure patient safety and comfort. AiMeds positioning products protect bony prominences and minimize nerve pressure while promoting circulation and respiratory function.